Northwest Colorado Community Health Center
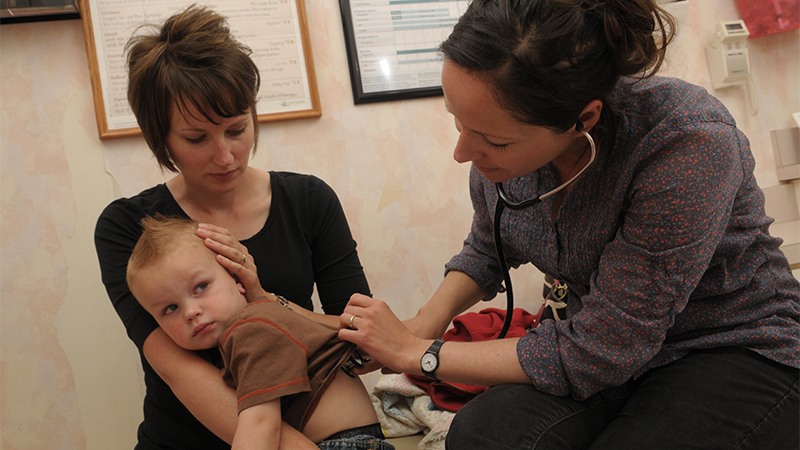
Photo by David Cornwell
By Sabine Kortals
The 9-year-old had never seen a dentist. The 3-year-old had speech delays that could be reversed with early intervention. The 7-year-old needed long-term counseling after finding her drug-addicted mother dead.
Just three years ago, these children had nowhere to turn.
In the remote ranching community of Craig, the safety-net clinic used to be open just two days a month. An extension of the local hospital, the clinic was struggling and rarely saw children.
“We wouldn’t even see sick children. We had to tell parents to go to the ER or go somewhere else,” said Diane Miller, Director of Clinical and Quality Services for the Northwest Colorado Health (NCH).
The NCH took over the clinic and successfully mounted a massive effort to win designation as a Federally Qualified Health Center in 2008.
One by one, new providers joined the clinic. First, there were enough to see patients two days a week. Now the Northwest Colorado Community Health Center boasts a full-time staff of medical and behavioral health experts and is open five days a week, including late hours on Monday evening. Everyone in the community is welcome, and providers can finally encourage families to seek preventive care.
“If you don’t have open spaces, you just have no way to address the health care needs of children,” Miller said.
Once the doors opened, providers discovered vast pockets of people who had gotten by without regular care. They ranged from children who had never had well-child checkups, immunizations and developmental screenings to teens suffering from depression in the area, which has disproportionately high suicide rates.
Clinic workers contended with some parents who would never dream of bringing a healthy child to a doctor.
“It’s really an Old West mentality of being able to deal with your problems on your own, not wanting government interference and not being dependent on anybody,” said Gisela Garrison, Health Center Director. “People think, you are healthy, you don’t need to go to a doctor, period. Only if you are really, really sick—almost dying—or if you had an accident. Then you go to the ER.”
Now, clinic workers are winning over families. Every time a child comes for an urgent matter, like an ear infection, doctors encourage parents to schedule their child’s next check-up.
Jennifer Mora is the clinic’s newest provider. A nurse practitioner, Mora started working at the clinic last summer with funding from The Colorado Trust. She gently encourages reluctant parents to follow up on care. For instance, when a mother of a 3-year-old wasn’t sure she wanted her child tested for speech delays, Mora reassured the mother.
“If you have your child screened now, you might find you won’t need help. Or, if therapy is needed, your child will get a better start now instead of falling behind,” Mora told the mom.
She also acknowledged her own experience with her 2-year-old’s speech. “I’ve gone through this myself. It’s not an unpleasant process,” Mora said.
Integrated behavioral health specialists also prove invaluable. When an 8-year-old girl came in recently suffering headaches after a car accident a month earlier, Mora knew the patient needed counseling, too. The girl was afraid to ride in a car, a paralyzing liability in this remote area.
“I told her it was OK to be afraid, that it was a really scary experience,” Mora said. Then, she was able to bring the counselor in to see the girl immediately.
With each child that the Craig clinic helps, providers plant a healing seed that builds trust and brings families back. “We’re trying to reach people before they get sick,” said Sue Birch, Chief Executive Director of the Northwest Colorado Health. “We’re trying to spin it all so we create an integrated community system that focuses on well-being.”